What is Diabetes?
Diabetes mellitus is a condition where blood sugar (glucose) levels are higher than normal. This happens because of a lack of insulin, or because the body does not use insulin properly.
The two main types of diabetes are:
Although both conditions result in high blood glucose, their causes, onset, affected population and treatment are significantly different. Understanding which type a person has is essential for safe and effective treatment.
Tests Diagnose Diabetes — They Don't Tell the Type
This is one of the most important points to understand about diabetes.
What is Type 1 Diabetes?
Type 1 diabetes is an autoimmune condition. The body's immune system mistakenly attacks and destroys the insulin-producing beta cells in the pancreas.
The result is very little or no insulin production, which causes blood sugar to rise rapidly.
Common Features of Type 1 Diabetes
- Often occurs in children or young adults — but can occur at any age
- Sudden onset — symptoms develop over days to weeks
- Frequent urination and excessive thirst
- Unexplained weight loss
- May present with diabetic ketoacidosis (DKA) — a medical emergency
Treatment of Type 1 Diabetes
What is Type 2 Diabetes?
Type 2 diabetes is caused by insulin resistance — the body does not respond properly to insulin — combined with a gradual decline in insulin production over time. It is the most common form of diabetes worldwide.
Common Features of Type 2 Diabetes
- Usually occurs in adults — but increasingly seen in younger people
- Gradual onset — often no symptoms in the early stages
- Often associated with overweight or obesity
- Strong family history is a common risk factor
- Frequently discovered during routine health screening
Treatment of Type 2 Diabetes
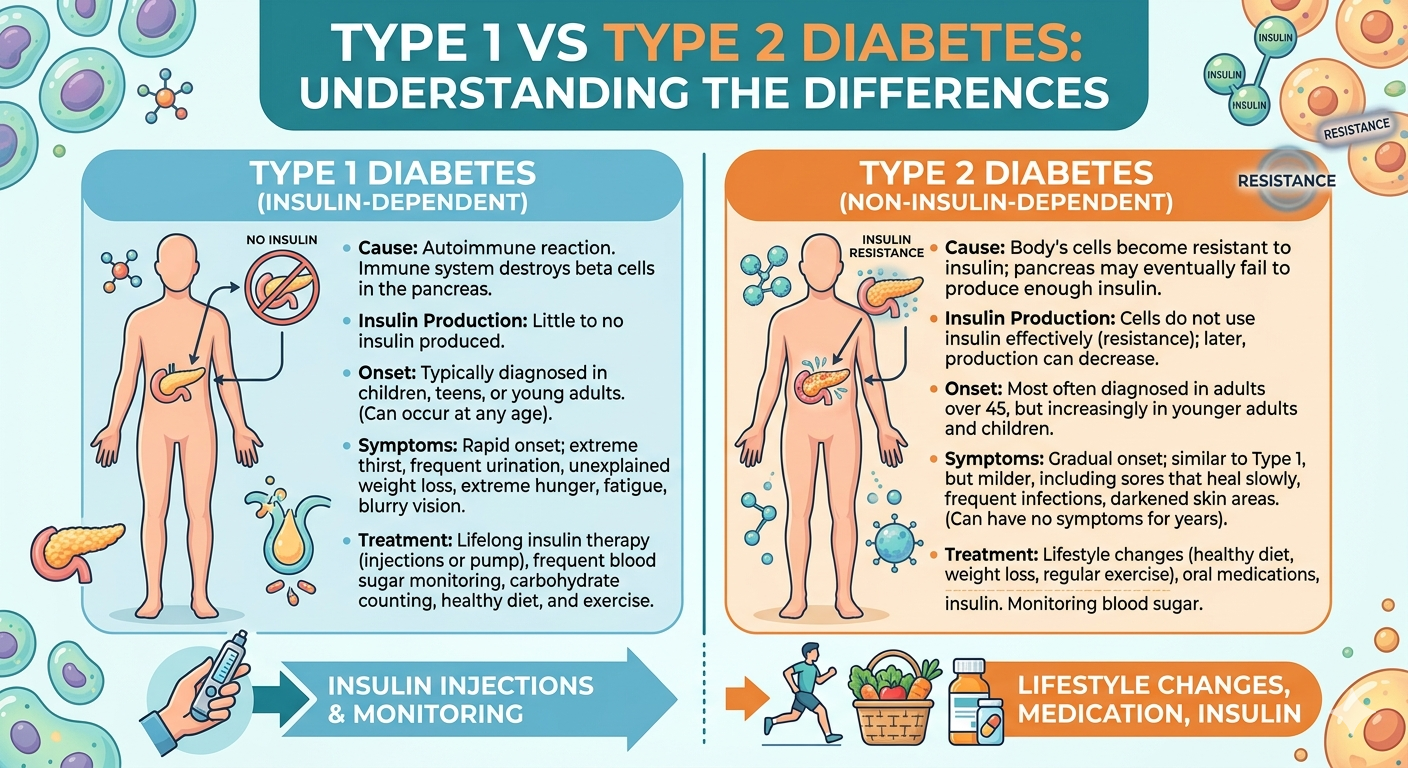
Type 1 vs Type 2: Key Differences
The table below summarises the most important differences between the two types of diabetes.
| Feature | Type 1 Diabetes | Type 2 Diabetes |
|---|---|---|
| Cause | Autoimmune destruction of insulin-producing cells | Insulin resistance ± gradual decline in insulin production |
| Onset | Sudden (days to weeks) | Gradual (months to years) |
| Typical age | Often children / young adults (any age possible) | Usually adults (increasingly in younger people) |
| Body weight | Often lean | Often overweight or obese |
| Insulin production | Very low or absent | Normal initially → declines over time |
| Treatment | Insulin required (lifelong) | Lifestyle changes ± oral tablets ± insulin |
How Do Doctors Confirm the Type?
After confirming the diagnosis of diabetes, doctors determine the type based on several factors:
1. Clinical Assessment (Most Important)
The most important step is a careful clinical assessment — the doctor considers:
2. C-Peptide Test
The C-peptide test measures how much insulin your own body is producing.
- 🔻Low C-peptide → suggests Type 1 diabetes (very little insulin production)
- ✅Normal or high C-peptide → suggests Type 2 diabetes (body still producing insulin)
3. Autoantibody Tests
Autoantibodies in the blood indicate that an autoimmune process is causing the diabetes. The most commonly tested are:
- GAD antibodies (Glutamic Acid Decarboxylase antibodies)
- Islet cell antibodies (ICA)
A positive autoantibody test strongly suggests Type 1 diabetes or LADA, even if the presentation initially appeared like Type 2.
Important Special Situations
LADA — Latent Autoimmune Diabetes in Adults
LADA is a form of autoimmune diabetes that initially appears similar to Type 2. However, it is actually caused by the same autoimmune process as Type 1 diabetes — just progressing more slowly.
- 🔍Often initially misdiagnosed as Type 2 diabetes
- 🕐Progresses gradually to insulin dependence over months to years
- 🧪Confirmed by positive autoantibody tests (GAD antibodies)
Lean Type 2 Diabetes
Not all people with Type 2 diabetes are overweight. Lean Type 2 diabetes occurs in individuals who are not obese and is relatively common in South Asian populations, including Sri Lanka.
Why Correct Classification Matters
Getting the type of diabetes right is not just an academic exercise — it has direct consequences for a patient's safety and health outcomes.
- Delayed insulin in Type 1 → life-threatening diabetic ketoacidosis (DKA) and dangerous complications
- Inappropriate treatment in Type 2 → poor glucose control and avoidable complications
- Misclassification of LADA → patient fails on tablets alone and eventually presents in crisis
When Should You Suspect Type 1 Diabetes?
When Should You Suspect Type 2 Diabetes?
Common Myths About Diabetes
Misinformation about diabetes is very common and can delay proper care. Here are the most important myths to correct:
- "Only older people get diabetes" — Type 1 commonly affects children and young adults. Type 2 is also increasingly seen in younger people.
- "Thin people cannot get Type 2 diabetes" — Lean Type 2 diabetes is real and relatively common, especially in South Asian populations.
- "All diabetes is the same" — The two main types have different causes, different risks, and require different treatment approaches.
- "Needing insulin means the disease is severe" — Insulin is essential for survival in Type 1 from the very start. Some Type 2 patients also need insulin as part of effective disease management — this does not mean their condition has suddenly worsened.
Frequently Asked Questions
- A healthy, balanced diet with reduced sugar and refined carbohydrates
- Regular physical activity (at least 150 minutes per week)
- Maintaining a healthy body weight
